Nobody prepares for this word.
The dentist says ‘pulpotomy’ and something tightens in your chest before your brain has even parsed the syllables. Surgical-sounding. Alarming. Definitely not a word that belongs in the same conversation as a six-year-old who still loses socks.
You catch maybe half of what the dentist says next. The rest is lost to the part of your brain already at home, typing that word into a search.
Here is what the search engine will not surface in the first thirty seconds: a pulpotomy is not a root canal. It is not as invasive as it sounds. And in the specific clinical situation where it gets recommended, it is usually the most sensible option on the table.
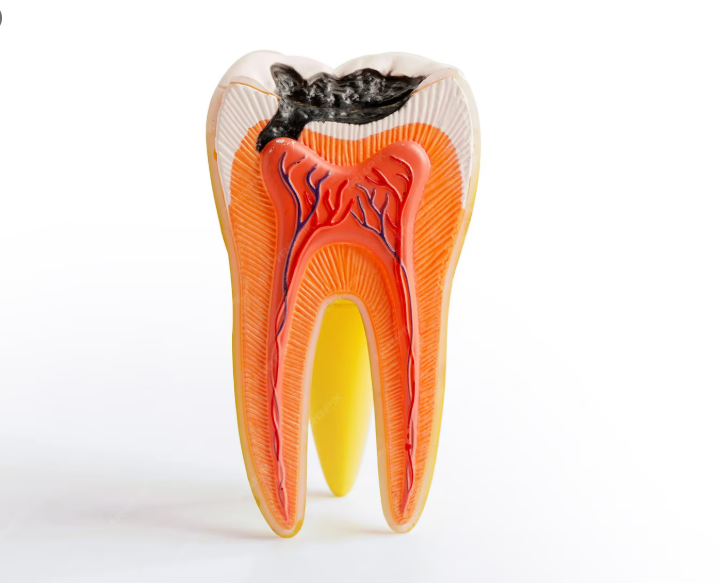
What the procedure actually does: removes the infected pulp tissue from the crown portion of the tooth only — not the root — treats what remains, and seals the tooth so it stays in the mouth, holds its space, and keeps doing its job until it is ready to fall out. The root stays. The tooth stays. The permanent tooth developing beneath it stays out of harm’s way.
This guide covers the reason the recommendation is made, what happens in the chair, what the material questions actually mean, what recovery involves, and what the success numbers say. By the end of it, the decision should feel like yours.
Baby Teeth Are Not Permanent. Neither Is Your Window to Save Them.
Decay in primary teeth moves faster than most parents expect. Significantly faster.
Baby teeth have thinner enamel and a much shorter distance from outer surface to pulp — the living tissue with the nerve. A cavity that might spend years approaching the nerve in an adult molar can reach it in months in a child’s tooth. And once it reaches the pulp, the infection does not stay contained.
It spreads through the root canals into the surrounding jawbone. Down into the tissue where the permanent tooth bud is already forming. An untreated pulp infection in a baby tooth can reach the adult tooth that is still years away from erupting.
This is why the recommendation comes quickly.
A pulpotomy is recommended at exactly the point where decay has reached the pulp but the root pulp is still healthy. The window is open. The procedure removes the infected coronal pulp, treats the remaining root tissue to stop the infection, and seals the tooth. The tooth holds its space. The permanent tooth underneath stays protected.
If that window is not used: extraction, and the cascade of space-loss consequences that come with losing a molar early. Or the infection is left to progress, which is worse. Neither of those is a better outcome than a forty-five minute appointment.
The timing of the recommendation is not dentist alarmism. It is the biology of primary teeth.
Where This Sits in the Treatment Spectrum — Because the Dentist May Not Have Explained It
Pulpotomy belongs to a treatment family called vital pulp therapy — procedures built around the principle of preserving living pulp tissue rather than removing it entirely. The specific procedure depends on exactly how far the decay has progressed.
Very close to the pulp but not there yet: indirect pulp cap. The deepest layer of decay is left in place, sealed and monitored rather than removed, to avoid exposing the pulp during excavation.
Just reached the pulp but the damage is minimal: direct pulp cap. A protective material is placed directly over the tiny exposure point.
Coronal pulp infected or inflamed, root pulp still healthy: this procedure. The infected upper tissue is removed, the root portion is treated, the tooth is restored.
Infection in the root canals: pulpectomy — full root canal on a baby tooth, more complex, occasionally appropriate — or extraction.
Decay reaching the coronal pulp of a primary molar with healthy roots is simply the most common presentation. The tooth is in exactly the window these procedures are designed for. Preserve what is preservable, for as long as it is preservable. That is the logic of vital pulp therapy.
Formocresol: The Thing Parents Google After the Appointment
After the infected tissue is removed, the root pulp needs to be treated with a medicament — a material that stabilises the tissue and prevents further bacterial activity. This is where most of the parental research happens, usually at home, after the appointment, when the word that surfaces is:
Formocresol.
It contains formaldehyde. That word produces a specific kind of alarm. Here is what the evidence actually shows: the amount of formaldehyde absorbed systemically during this procedure is extremely small. Smaller than the formaldehyde the human body produces through normal daily metabolism. Smaller than the exposure from common household products. The safety record runs over a century. The harm the midnight search implies has not been demonstrated.
Alternatives exist and are widely used: mineral trioxide aggregate, ferric sulfate, biodentine — each with strong clinical evidence. If the material matters, ask the dentist before the appointment which one they use and why. A direct question that deserves a direct answer.
On outcomes: the success rate for primary molar treatment with this procedure sits consistently between eighty-five and ninety-five percent across materials and study populations. That number holds regardless of which medicament is used.
What Actually Happens. In the Chair. Step by Step.
From the child’s point of view: tooth numbed, something happens, silver cap. That is typically the full summary. With good anaesthesia and a well-run clinical environment, most children tolerate it without significant distress.
From the clinical side, four stages:
One: Anaesthesia. Local anaesthetic is administered. The tooth and surrounding tissue go completely numb. A rubber dam — a thin sheet of latex or latex-free material — isolates the tooth and keeps the working area dry. The child feels pressure throughout. They should feel no pain. If they signal pain, the procedure stops. More anaesthetic goes in. Nothing continues until the area is completely numb.
Two: Pulp removal. The roof of the pulp chamber is opened and the coronal pulp removed. The chamber is cleaned and the bleeding at the canal openings assessed. Controlled, minimal bleeding means the root pulp below is healthy and the procedure can proceed as planned. Heavy or uncontrolled bleeding means infection may have already reached the root canals — the treatment plan changes.
Three: Medicament. The chosen material is applied to the root pulp tissue at the canal openings. A base material — typically zinc oxide eugenol or equivalent — seals the pulp chamber above it.
Four: The crown. A stainless steel crown is placed in almost every case. This is not optional and it is not cosmetic. A tooth that has been opened to this depth, had its coronal pulp removed, and had the chamber sealed does not have the structural integrity to survive normal chewing force with just a filling on top. The crown is why the tooth can stay in service until it falls out naturally.
Total appointment time: forty-five minutes to an hour, including getting the child settled.
The Silver Crown: What It Is, Why It Is There, When It Leaves
The post-appointment concern almost always transfers to the crown. It is silver. It is visible. It was not in the plan anyone had for their child’s mouth.
Teeth restored with full crowns after this procedure outlast those restored with composite fillings. Consistently. The procedure leaves the tooth structurally compromised. A filling does not fix that. The crown does.
On visibility: back molars, which is where most of these procedures are performed, are not visible when a child talks or smiles. They are visible when a child opens wide. For front teeth, tooth-coloured crown options exist where clinically appropriate.
On permanence: the crown leaves with the tooth. When the baby tooth exfoliates naturally, the crown comes out with it. There is nothing to remove separately.
Most children forget about it within days. Parents take longer.
Recovery: The Anaesthetic Is the First Thing to Manage
The most predictable post-appointment problem is not pain from the procedure. It is the anaesthetic.
The numbing takes one to three hours to clear. During that window the cheek, lip, and tongue feel strange. Children do not always connect the odd sensation to the instruction not to bite. Some chew the inside of their cheek without realising. The result is soft tissue ulceration that can look alarming and takes several days to resolve.
Watch specifically for this in the two hours after the appointment. Soft food during this window reduces the likelihood considerably.
Once the anaesthetic is fully gone: mild to moderate soreness at the injection site and around the tooth is expected. It is tissue responding to the procedure, not a sign that something failed. Children’s paracetamol at the weight-appropriate dose handles it reliably. Most children have no remaining awareness of the tooth beyond the first twenty-four hours.
Call the dental practice if:
• Pain is increasing at 48 hours rather than settling
• Swelling appears in the gum, jaw, or face beyond the immediate area
• Fever develops in the 24 to 48 hours after the procedure
• The crown feels raised and the child is biting unevenly
• The crown comes loose or falls off in the first week
After the first few days, the crown is just part of the mouth. Brushing and flossing around it continues exactly as before. The child will not mention the tooth again until a dentist brings it up.
How Well Does a Pulpotomy Work? The Number Worth Knowing.
It is one of the most studied procedures in paediatric dentistry.
Clinical success — the tooth surviving without further intervention until natural exfoliation — is documented consistently between eighty-five and ninety-five percent. For a tooth that the alternative treatment would have extracted, that is a strong outcome.
The ten to fifteen percent that does not succeed: the majority of these failures appear on X-ray before the child has any symptoms. Pathological root resorption — the bone around the root eroding as infection continues beneath the treated tissue — shows up radiographically before it becomes clinically apparent. This is why follow-up dental visits are not optional after this procedure. The X-ray monitoring is not a formality. It is part of the treatment.
When a treated tooth eventually fails: pulpectomy occasionally, or extraction with a space maintainer to hold the gap.
A tooth that later needs extraction was not a treatment failure. Biological processes are not fully predictable. The monitoring exists to catch those cases early, before symptoms develop.
The Procedure Is Straightforward. The Setting Is Not Irrelevant.
The clinical steps of a pulpotomy on a primary tooth are not complicated. What surrounds those steps is where the appointment can go wrong.
A four-year-old in a dental chair has a limited cooperation window, a limited ability to describe discomfort, and a genuine chance of anxiety at some point. Whether the appointment is manageable or frightening depends almost entirely on the clinical environment and the people in it.
For families in the UAE, access is not the obstacle. Medical & Dental Services in Dubai includes specialist paediatric centres staffed for exactly this on young children. A well-established Dental & Medical Center with paediatric specialists integrates the procedure with appropriate pre-assessment, anaesthesia calibrated to the child’s age, and follow-up monitoring. Families in International City Dubai and nearby areas have access to multi-specialty centres where paediatric dental care sits within a broader child health context — relevant when health considerations affect anaesthesia.
The sedation conversation — whether nitrous oxide or oral sedation is appropriate — should happen before the appointment, not during it. It is a conversation about the specific child: their age, their anxiety history, their triggers. A practice that offers sedation options and deploys them regularly is a different environment for an anxious child than one that offers them reluctantly or not at all.
Questions Parents Actually Ask
Not the composed ones. The ones people type at 11pm.
Is my child going to be in pain?
Not during. Local anaesthesia numbs the area completely — the tooth, the gum, the surrounding tissue. The child feels pressure. They should not feel pain. If they signal pain, the procedure stops until more anaesthetic is in. After: mild soreness for a day or two, handled with children’s paracetamol. Most children have forgotten about the tooth entirely by the next morning.
It’s a baby tooth. Why not just take it out?
Because the space does not stay empty. Baby molars are holding a gap that the permanent molar will not fill for years. When a primary molar is lost too early, the teeth on either side drift in. The permanent molar arrives with no room. Crowding follows. Orthodontic treatment at twelve or thirteen follows that. If the tooth can be saved, saving it avoids a problem that extraction starts. That is the whole logic of the recommendation.
What is formocresol and why does it alarm me?
It contains formaldehyde — that is the part that produces alarm when people research it. The evidence shows systemic absorption from this procedure is extremely small — lower than what the body produces daily through normal metabolism, and well below typical household exposures. The safety record in paediatric dental practice is over a century long. Alternatives with strong evidence exist: mineral trioxide aggregate, ferric sulfate, biodentine. Ask the dentist which material they use and why — before the appointment, not after.
Will this damage the adult tooth growing underneath?
Correctly performed and monitored, the procedure protects the adult tooth. The whole reason to act at this stage is that untreated pulp infection spreading into the jawbone — where the permanent tooth bud is developing — is what damages permanent teeth. The procedure stops the infection from reaching that tissue. Not treating is the risk. The procedure contains it.
My child is already anxious about dentists. Will this make everything worse?
Not if the environment handles it well. Tell-show-do, appointment pacing, nitrous oxide, oral sedation — standard tools in a specialist setting. Have the conversation with the practice before the appointment: what does this child need? A practice that manages anxious children routinely has seen worse than yours.
How do I know if it worked?
In the short term: the crown is stable, the child is not in pain beyond the first couple of days, eating is normal. Over time: follow-up X-rays at subsequent dental visits check for pathological root resorption, the main indicator of failure. Success builds as a picture across multiple appointments. It is not confirmed in a single visit. Attending the follow-up appointments is not optional — that is how failure gets caught before it becomes a bigger problem.
What does this cost in Dubai, and will insurance actually cover it?
Costs vary by clinic and by whether sedation is involved. The fee typically covers the procedure, the crown, and the X-rays taken beforehand. Most UAE health plans include paediatric dental procedures, though some require pre-authorisation for more complex treatments. Confirm coverage with both the insurer and the clinic before the appointment.