You did not choose this. The tooth did.
At some point in a recent dental appointment, the dentist tilted a screen toward you, pointed at something in your jaw, and started explaining. You followed the first thirty seconds. Then the words ‘impacted’ and ‘surgical’ appeared together and something in your brain filed the rest of the conversation under ‘deal with this later.’
Later is now. This is what a surgical extraction of an impacted wisdom tooth actually involves — why leaving it in is not safe, what the procedure does to get it out, what recovery genuinely looks like (not the version calibrated to keep you calm), what can go wrong, and what to ask your surgeon before you agree to anything.
By the end of this, the appointment should feel like something you chose. Not something that happened to you while you nodded along.
The Tooth Is Not Going to Quietly Settle Down. It Has Been Proven Not To.
People want this to be a wait-and-see situation. It is not.
An impacted wisdom tooth — one that cannot erupt because there is no space, the angle is wrong, or another tooth is in the path — does not negotiate its way into a stable position over time. It stays stuck. Stuck teeth are not harmless teeth.
Infection comes first, usually. The partially erupted tooth creates a gum flap that collects food and bacteria. The infection — pericoronitis — is not subtle. Pain, swelling, sometimes a jaw that will not open fully. Antibiotics clear it temporarily. Then it comes back. It keeps coming back until the tooth is gone.
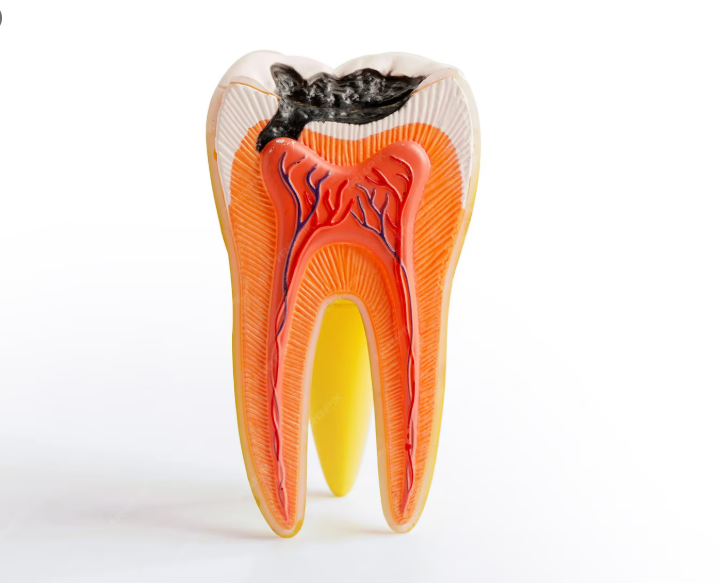
Decay is quieter. A wisdom tooth pressing against the molar in front creates a contact point impossible to clean. Decay builds on both surfaces with no pain until it is well advanced. By the time it appears on an X-ray, it has usually been there a while. The molar being pressed on — worth considerably more than the wisdom tooth — is the one that ends up damaged.
Root resorption, cysts, front-tooth crowding: less common. Also documented. Also not on a trajectory toward self-resolution.
The case for surgical extraction is not dentists being conservative. It is the documented outcome of leaving these teeth in place.
It Is Called Surgical Because There Is Cutting. Here Is Exactly What That Means.
A standard extraction works on a tooth that is already above the gum: grip it, work it loose, remove it through the socket. An impacted tooth is not above the gum. It is not accessible. That approach does not apply.
A surgical extraction starts with an incision. The gum tissue is cut and reflected back to expose the tooth and the bone covering it. Some of that bone is removed to gain access. The tooth is almost always sectioned — cut into two or three pieces — so that each section can be maneuvered out through the socket without the whole tooth needing to fit through an opening it never would have fit through intact.
Cut tissue heals. Worked bone responds. The socket left behind is larger. That is why day three catches people off guard.
Most people are awake for this. Local anaesthesia numbs the area completely — pressure and vibration throughout, no pain. Sedation is available at equipped clinics. Discuss it before the appointment, not on the day.
Thirty minutes to an hour for a straightforward impacted molar extraction. Deeper impactions, roots close to the inferior alveolar nerve, unusual angulation — these take longer. The pre-procedure conversation should tell you which category you are in.
The Consultation Before Is Not a Warm-Up. It Is Half the Work.
The appointment before the extraction is where most of the important decisions happen. Patients often treat it as paperwork. It is not paperwork.
The panoramic X-ray — OPG — shows all four wisdom teeth: position, depth, angulation, and root proximity to the inferior alveolar nerve. If the roots are very close, a cone beam CT adds three-dimensional detail. Not every case needs one. Ask specifically what the OPG shows about your tooth.
Medical history: blood thinners, clotting disorders, bisphosphonates, immunosuppression, diabetes — all affect how the procedure goes. Mention everything. What feels irrelevant often is not.
Pre-operative instructions: for local anaesthesia, eating restrictions usually do not apply. For sedation or general anaesthesia, fasting is required and is non-negotiable. The practice gives you specific instructions. Follow them exactly.
The night before: no alcohol. Have a driver arranged. Even with local anaesthesia only — no sedation at all — driving yourself home after is not advisable. Stress plus residual numbness is a bad combination behind a wheel. For sedation, someone driving you is a condition of the procedure.
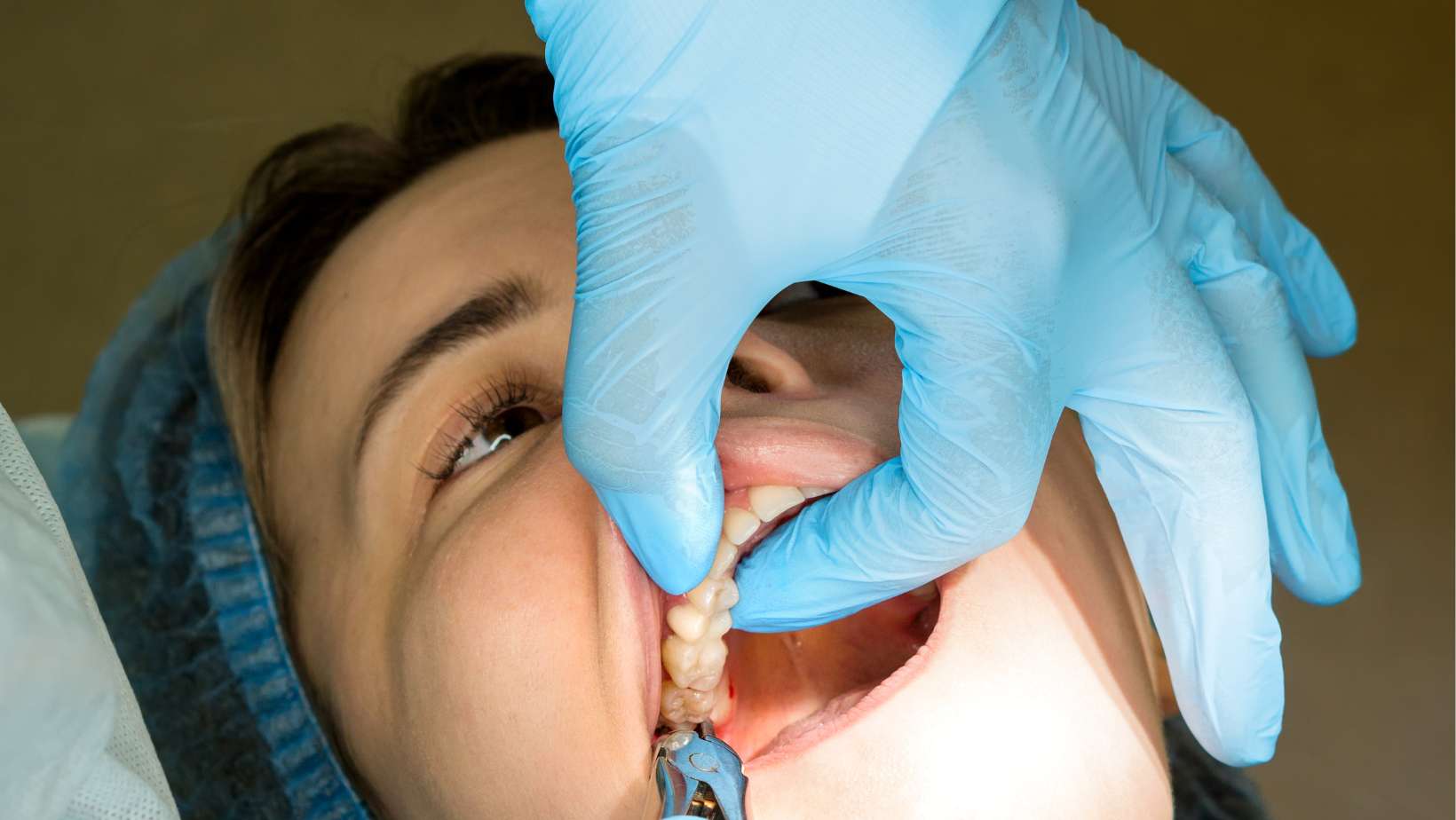
What Happens in the Chair — Everything, Including the Part About the Drill
What happens, in order:
Anaesthesia. Injected into the gum and the nerve block for that jaw region. Numbness takes a few minutes to set fully. You feel pressure and movement throughout the procedure — not pain. If you feel pain at any point, you say so. More anaesthetic goes in. The procedure does not continue until the area is completely numb.
Incision and reflection. Small cut in the gum. Flap reflected back to expose the tooth and the underlying bone. Pressure. Movement. No pain.
Bone removal. A drill removes the bone covering the tooth. Loudest part of the procedure. Vibration through the jaw — significant but not painful. It will startle you if nobody mentioned it was coming. Now you know.
Sectioning and removal. The tooth is cut into sections and each piece removed individually. Less force, better access, lower risk to adjacent structures.
Suturing. Gum flap sutured back. Resorbable sutures dissolve at seven to ten days. Non-resorbable ones require a short follow-up visit to remove. Ask which type was used before you leave.
Read the post-operative instructions before the anaesthetic fully wears off. Not the next morning when the pain has already arrived.
Recovery: Day One Is Fine. Day Three Is the One Nobody Warned You About.
Day one: manageable. The anaesthetic is wearing off, there is some bleeding, some swelling starting. Most people are surprised it is not worse.
Day three: the one that actually surprises people. Swelling peaks at 48 to 72 hours. The face looks different. The jaw is stiff. Opening the mouth takes effort. This is expected. It is not a sign something went wrong. It is just what soft tissue and bone do when they are healing from a procedure of this size.
Day seven: functional. Most people are eating reasonably normally, the swelling has dropped significantly, and the pain is manageable without the stronger analgesics.
Day fourteen: most people have stopped thinking about it.
First 24 hours — the rules that actually matter:
Bite on the gauze. Maintain pressure. Bleeding for a few hours is normal. No spitting, no straws, no forceful rinsing, no smoking — each one dislodges the clot forming in the socket. That clot is how healing starts. Lose it and you get dry socket, which is more painful than the surgery itself.
Ice to the face in twenty-minute intervals for the first 24 hours. After that, heat works better.
Pain once numbness clears: take analgesics proactively, as prescribed. Do not wait until it is unbearable.
Days two to four:
Soft food only. Salt water rinses gently after meals from day two. No alcohol-based mouthwash for the first week. Jaw stiffness and limited opening are both normal and both temporary.
Days five to fourteen:
Progressive improvement. Normal eating around day seven to ten. Keep the socket clean. Sutures dissolve or are removed at seven to ten days.
Call the practice — do not wait and see — if:
• Pain is getting worse after day three instead of better
• There is a foul taste or smell coming from the socket — that is dry socket
• Fever above 38°C after the first 24 hours
• Numbness or altered sensation in the lip, chin, or tongue that has not cleared by the day after surgery
• Swelling still increasing past day four
• Bleeding that will not stop with sustained pressure after two hours
Surgical Teeth Removal and the Complications: Not Rare Enough to Skip This Section
Most surgical teeth removal procedures heal without incident. Knowing what the complications look like means you catch them early.
Dry socket:
Three to five percent of extractions overall; up to thirty percent after lower wisdom tooth removal. Bone is exposed, and a distinctive throbbing pain starts three to five days post-procedure — it does not respond to standard pain relief, which is how you identify it. Treated with medicated socket dressing. Smoking is the largest avoidable cause.
Nerve disturbance:
The inferior alveolar nerve runs close to the roots of lower wisdom teeth. Temporary altered sensation in the lower lip, chin, or teeth on that side is a known risk of impacted molar extraction — resolves over weeks to months in the majority of cases. Permanent altered sensation is uncommon. The pre-operative X-ray maps exactly how close your roots sit to that nerve.
Infection:
Increasing pain and swelling after day three, pus, fever. Most post-surgical infections respond to a course of antibiotics. Prophylactic antibiotics are not routine for straightforward cases but are prescribed when the risk profile warrants it.
Damage to the adjacent tooth:
Rare. More likely when the wisdom tooth has been pressing against the second molar for a long time or the roots are intertwined. A surgeon who does this regularly keeps this risk very low. Not zero.
Before an Impacted Molar Extraction: Ask the One Question Most People Forget
Not the cost. Not how long it takes.
The question is: what is the actual risk level of this specific tooth?
A partially erupted tooth tilted slightly forward is a different clinical scenario from a deeply bony-impacted tooth with roots curving around the inferior alveolar nerve canal. Both are called impacted wisdom teeth. They are not the same procedure.
Your X-ray shows the surgeon exactly which situation they are dealing with. You are allowed to see it. You are allowed to ask about it. These are the specific questions worth asking:
• How close are the roots to the inferior alveolar nerve?
• Will the tooth need to be sectioned?
• Is this a routine case or a complex one?
• How many cases at this difficulty level have you performed?
A surgeon who does this regularly will answer all four without hesitating. Hesitation on any of them is information.
On timing: easier to remove at twenty-two than at thirty-five. Softer bone, less developed roots, faster recovery. People who wait for symptoms do not have an easier experience — they have a later, more complicated one.
Where You Have This Done Is a Clinical Variable, Not a Preference
The steps of the procedure are standard. Who is executing them — and how many times they have done it — is not.
A surgeon who performs surgical extractions routinely has encountered the full range: easy cases, difficult ones that turned mid-procedure, nerve proximity, patients struggling with the sounds and pressure. None of it is new to them. The response is practiced.
A dentist who removes wisdom teeth occasionally has the same training but a narrower bank of real experience behind each decision. That does not matter on a straightforward day. It matters significantly when the case turns out to be more complex than expected. Which does happen.
For patients in the UAE, specialist access is real. Medical & Dental Services in Dubai includes oral and maxillofacial surgery practices where surgical extraction is part of the regular caseload. A well-equipped Dental & Medical Center with an oral surgeon on staff can assess the full complexity, discuss sedation properly, perform the procedure, and follow up post-operatively. Patients in International City Dubai and surrounding areas have multi-specialty centres where surgical dental care sits alongside broader medical services — relevant when health conditions affect anaesthesia planning.
If anxiety is real, raise it before the appointment. Nitrous oxide, IV sedation, and general anaesthesia are available in equipped settings.
What People Are Actually Asking Before They Book
The questions people type at midnight. With direct answers.
Be honest — how bad is the pain?
During: none. The area is completely numb. Pressure, movement, vibration from the drill — not pain. If you feel pain, say so. Nothing continues until more anaesthetic goes in. After: real pain, yes, for two to four days. Take analgesics before the pain builds, not after it does. Day three is typically the worst. By day seven most people are considerably better. By day fourteen most have stopped taking anything.
Do all four really have to come out? Right now?
Not all four, not always at once. Some surgeons prefer one session under sedation; others stage them. Depends on how many are impacted, how complex each one is, your health. Ask what the surgeon recommends for your case.
How long before my life is normal again?
Two to three days off work for a routine case. No physical activity for the first week. Normal eating around day seven to ten. Fully functional by day fourteen for most people. If sedation or multiple teeth are involved, plan longer. The people who plan for one day and need four feel blindsided.
What is dry socket and why does everyone say it like it is the worst thing?
Because it is worse than the surgery. The clot in the socket is disrupted before healing tissue forms beneath it. Bone is exposed. A distinctive throbbing pain starts three to five days post-procedure and does not respond to standard pain relief — that unresponsiveness is how you recognise it. Treated with medicated dressing at the practice. To avoid it: no smoking, no straws, no forceful spitting or rinsing in the first 48 hours. Not dangerous. Just considerably more painful than anyone expects.
I read something about nerve damage and now I cannot stop thinking about it.
For most people, this is not the outcome. Disturbance during surgical teeth removal can cause temporary numbness in the lower lip, chin, or teeth on that side — resolving over weeks to months in most cases. Permanent altered sensation is uncommon. Ask your surgeon specifically how close your roots are to the nerve canal on your X-ray. If the proximity is significant, a cone beam CT provides better detail. You are entitled to a specific answer before you consent.
Honestly, it does not hurt at all right now. Does it actually need to come out?
Asymptomatic does not mean stable. A horizontally impacted tooth pressing against the second molar is causing damage whether you feel it or not. Pericoronitis comes back. Adjacent molar decay builds silently. Earlier removal means a simpler procedure and faster recovery. Base the decision on the X-ray, not on how it feels today.
What does this cost in Dubai and will my insurance cover it?
Cost varies by complexity and whether sedation is involved. Most UAE health insurance plans include oral surgery, but pre-authorisation is often required and coverage levels vary. Get the specifics from insurer and clinic before booking. Practices that do this regularly will help with the documentation.